Understanding Perimenopause: The Hormonal Rollercoaster
Perimenopause, the transitional phase leading up to menopause, often begins in a woman’s 40s, though it can start earlier. During this time, ovarian function begins to decline, leading to fluctuating levels of estrogen and progesterone. This hormonal imbalance can manifest in various symptoms, including irregular periods, hot flashes, night sweats, mood swings, sleep disturbances, and a noticeable shift in metabolism.
Many women in perimenopause experience weight gain, particularly around the abdomen, even without significant changes to diet or exercise. This is often linked to declining estrogen affecting insulin sensitivity and fat distribution. Understanding these physiological shifts is crucial when exploring dietary interventions like intermittent fasting.

The Promise of Intermittent Fasting: A Brief Overview
Intermittent fasting (IF) is an eating pattern that cycles between periods of eating and voluntary fasting. It’s not about *what* you eat, but *when* you eat. Common benefits often associated with IF include weight management, improved insulin sensitivity, enhanced cellular repair processes (autophagy), and reduced inflammation. By giving the body regular breaks from digestion, IF encourages it to tap into fat stores for energy and can optimize metabolic function.
While IF has gained popularity for its broader health benefits, its application during the delicate hormonal phase of perimenopause requires a nuanced and individualized approach. The key is to support the body, not stress it further, during a time of significant physiological change.
Why Consider IF During Perimenopause?
For perimenopausal women, intermittent fasting may offer several potential benefits that align with common concerns during this life stage:
- Weight Management: Hormonal shifts often lead to a slower metabolism and increased fat storage, making weight loss more challenging. IF can help by improving insulin sensitivity, promoting fat burning, and reducing overall calorie intake naturally within eating windows.
- Improved Insulin Sensitivity: Estrogen decline can negatively impact insulin sensitivity, contributing to increased risk of type 2 diabetes and abdominal fat. IF helps stabilize blood sugar levels and can make cells more responsive to insulin.
- Reduced Inflammation: Chronic inflammation is linked to many age-related diseases and can exacerbate perimenopausal symptoms. IF has been shown to reduce inflammatory markers in the body.
- Cellular Repair (Autophagy): During fasting, the body initiates autophagy, a process where cells clean out damaged components and regenerate. This can promote cellular health and potentially slow aspects of aging.
- Enhanced Energy Levels: While initially some may experience fatigue, many report sustained energy and mental clarity once their body adapts to using fat for fuel.
Tailoring Intermittent Fasting Schedules for Perimenopausal Women
Given the hormonal sensitivity of perimenopausal women, a “one-size-fits-all” approach to intermittent fasting is not ideal. Starting gently and listening intently to your body is paramount. Here are several common intermittent fasting schedules, with considerations for perimenopausal women:
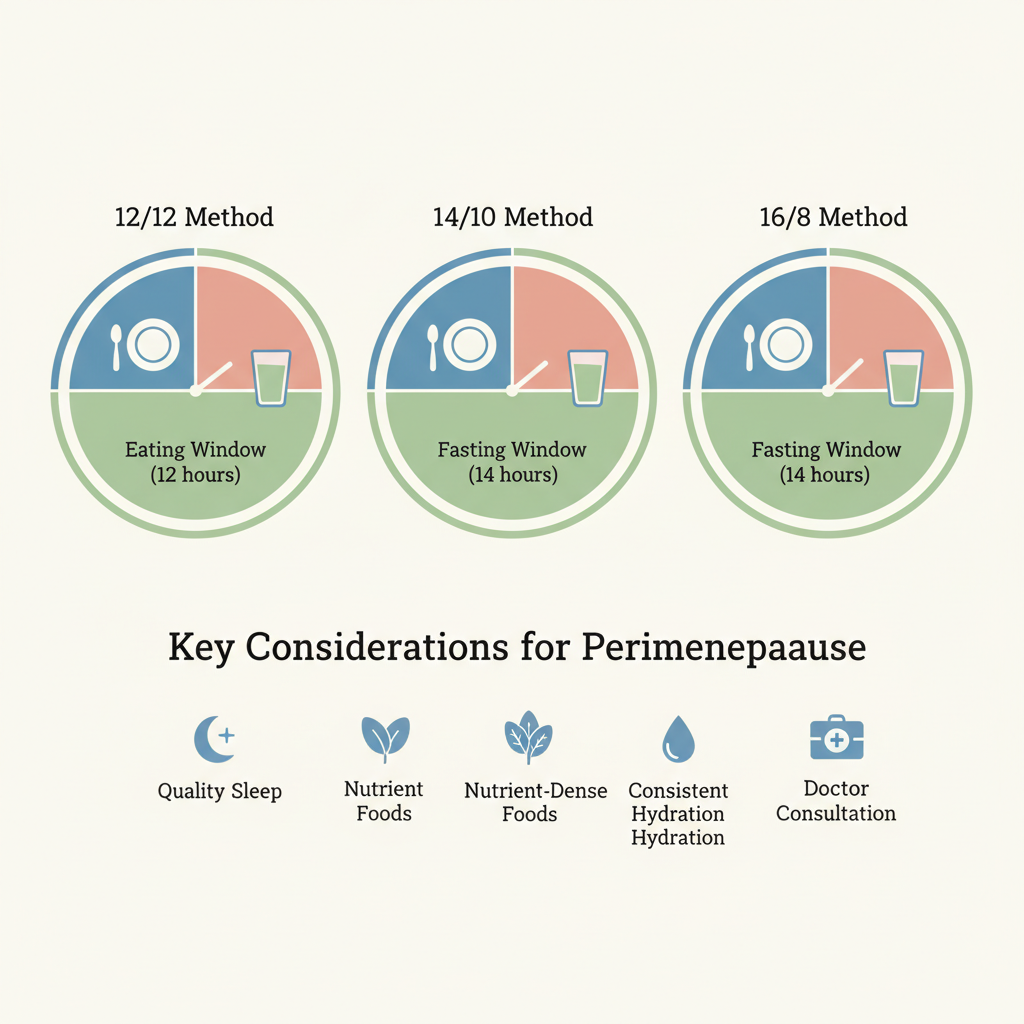
The Gentle Introduction: 12/12 Method
This is the most approachable form of IF and can be an excellent starting point. You fast for 12 hours and eat within a 12-hour window. For most, this simply means finishing dinner earlier and delaying breakfast slightly. For example, if you finish eating by 7 PM, you would have your first meal at 7 AM.
- Why it’s good for perimenopause: It minimizes stress on the body and hormones, allowing for metabolic benefits without extreme restriction. It can help regulate eating patterns and improve sleep without feeling deprived.
The Popular Choice: 14/10 or 16/8 Methods
The 14/10 method involves a 14-hour fast followed by a 10-hour eating window. The 16/8 method, often called the Leangains protocol, extends the fast to 16 hours, with an 8-hour eating window. These are popular choices for their effectiveness and flexibility.
- Why it’s good for perimenopause: Many perimenopausal women find the 14/10 method to be a sweet spot, offering metabolic benefits like improved insulin sensitivity and fat burning without being overly taxing on hormonal balance. The 16/8 method can also be effective but requires careful monitoring for signs of stress or fatigue.
- Adaptation tip: Consider skipping breakfast or delaying it until late morning, then having dinner in the early evening. Ensure your eating window includes nutrient-dense meals.
More Advanced Approaches: 5:2 and ADF (with caveats)
The 5:2 method involves eating normally for five days a week and severely restricting calories (typically 500-600) on two non-consecutive days. Alternate Day Fasting (ADF) involves fasting every other day, often with a small meal (around 500 calories) on fasting days.
- Why caution is needed for perimenopause: While effective for weight loss, these more restrictive methods can be more stressful for the female body, especially during perimenopause. They can potentially impact cortisol levels, worsen sleep, or exacerbate hormonal imbalances for some women.
- Recommendation: Approach these methods with extreme caution and only after adapting well to gentler schedules and consulting a healthcare professional. Listen closely to your body for any adverse reactions.
Key Considerations for Safe and Effective IF in Perimenopause
Successful intermittent fasting for perimenopausal women goes beyond just choosing a schedule. It requires a holistic approach:
Listen to Your Body First
This is the most critical advice. If you experience increased fatigue, irritability, insomnia, mood swings, or a worsening of hot flashes, it’s a sign that your chosen schedule might be too aggressive. Consider shortening your fasting window or taking a break. Your body’s signals are paramount.
Prioritize Nutrient-Dense Foods
During your eating window, focus on whole, unprocessed foods. Emphasize lean proteins, healthy fats (avocado, nuts, seeds, olive oil), complex carbohydrates (vegetables, whole grains), and plenty of fiber. These foods support satiety, provide essential nutrients, and help stabilize blood sugar, minimizing cravings.
Hydration and Electrolytes
Stay well-hydrated throughout the day, especially during fasting periods. Water, herbal teas, and black coffee are permissible. Consider adding a pinch of sea salt or electrolyte supplements if you experience headaches or muscle cramps, particularly during longer fasts.
Sleep and Stress Management
Adequate sleep is crucial for hormonal balance and metabolic health. Fasting can sometimes impact sleep for some women, so monitor this closely. Combine IF with stress-reducing practices like yoga, meditation, or spending time in nature. Chronic stress can counteract the benefits of IF by elevating cortisol.
Exercise Smartly
Maintain a consistent exercise routine, but avoid intense, prolonged workouts during longer fasting periods, especially when starting. Opt for moderate activities like walking, cycling, or strength training. High-intensity exercise combined with fasting can sometimes be an added stressor on the body.
Professional Guidance is Paramount
Before beginning any new dietary regimen, especially during perimenopause, consult with your doctor or a registered dietitian. They can assess your individual health status, consider any underlying conditions or medications, and help tailor a safe and effective plan that supports your unique needs.
Conclusion
Intermittent fasting can be a powerful tool for perimenopausal women seeking to manage weight, improve metabolic health, and alleviate some symptoms associated with hormonal shifts. However, success hinges on choosing the right schedule, prioritizing nutrient-dense foods, and, most importantly, listening to your body’s signals. Start gently with shorter fasting windows, be patient, and always seek professional medical advice to ensure your approach supports your health and well-being through this significant life stage.



