These flare-ups are essentially periods when your immune system becomes more active against your thyroid gland, intensifying symptoms like fatigue, brain fog, weight fluctuations, joint pain, and mood disturbances. Identifying and addressing these triggers is the cornerstone of effective Hashimoto’s management, moving beyond just medication to a holistic approach.
Understanding Hashimoto’s Thyroiditis and Flare-Ups
Hashimoto’s thyroiditis is an autoimmune condition where the immune system mistakenly attacks the thyroid gland. This chronic inflammation can eventually lead to an underactive thyroid (hypothyroidism), requiring lifelong hormone replacement therapy.

A “flare-up” signifies a period of increased autoimmune activity, often resulting in a worsening of hypothyroid symptoms or even transient hyperthyroid symptoms as the damaged thyroid tissue releases stored hormones. These episodes can be debilitating and frustrating, emphasizing the need to pinpoint their root causes.
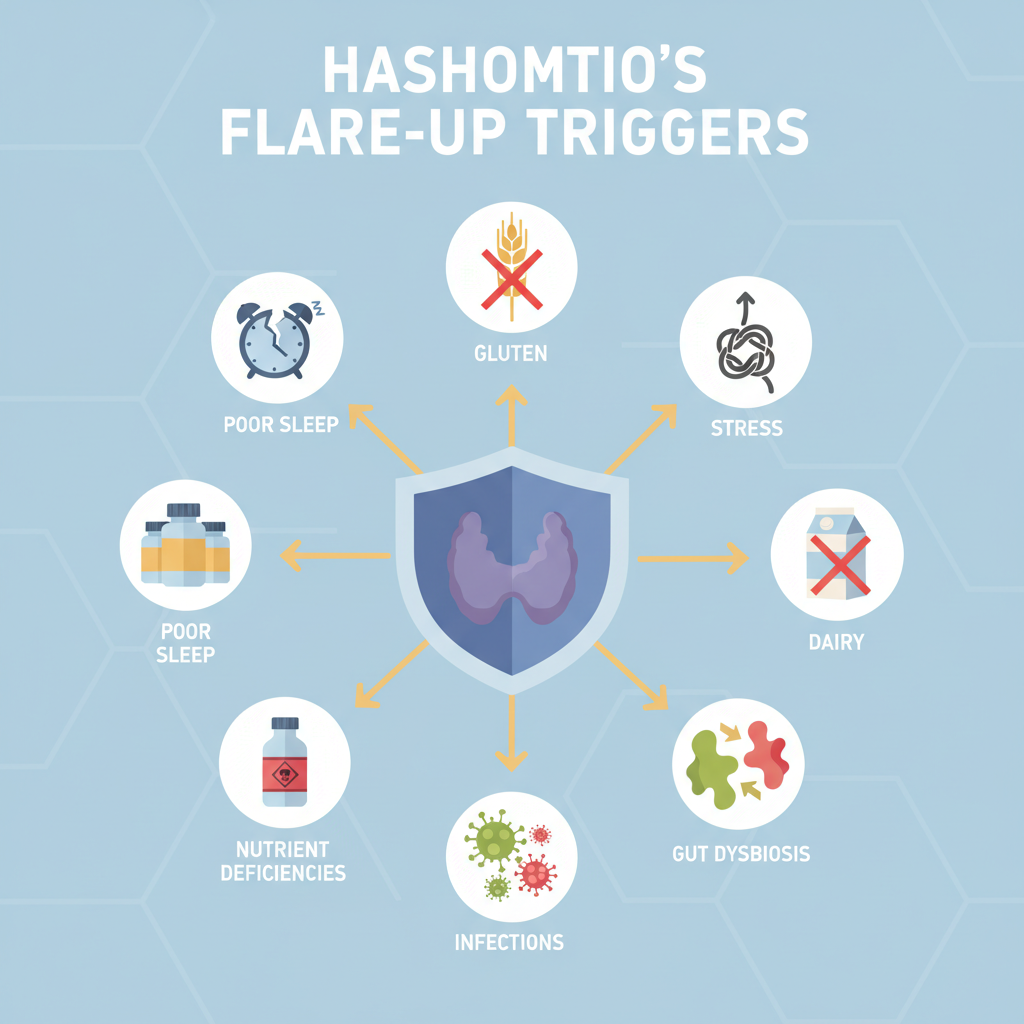
Common Hashimoto’s Thyroiditis Flare-Up Triggers
1. Chronic Stress and Emotional Strain
Stress is one of the most significant and pervasive triggers for autoimmune conditions, including Hashimoto’s. Chronic stress elevates cortisol levels, which can disrupt immune function and exacerbate inflammation. This constant pressure can create a vicious cycle, making the immune system more reactive.
Learning effective stress management techniques, such as mindfulness, meditation, deep breathing exercises, or engaging in hobbies, is not just about mental well-being; it’s a critical component of managing your autoimmune response and preventing flares.
2. Dietary Factors: Gluten, Dairy, and Inflammatory Foods
For many individuals with Hashimoto’s, certain foods can act as potent triggers. Gluten, a protein found in wheat, barley, and rye, is a common culprit due to a phenomenon called molecular mimicry, where the immune system confuses gluten with thyroid tissue.
Dairy products, particularly casein, can also provoke an inflammatory response in sensitive individuals. Furthermore, highly processed foods, excessive sugar, and unhealthy fats contribute to systemic inflammation, making the immune system more prone to attacking the thyroid. Exploring an elimination diet under professional guidance can help identify your specific food sensitivities.
3. Gut Health Imbalances (Dysbiosis & Leaky Gut)
The gut plays a pivotal role in immune system regulation. An imbalance in gut bacteria (dysbiosis) or increased intestinal permeability (often referred to as “leaky gut”) can allow undigested food particles and toxins to enter the bloodstream, triggering an immune response. This continuous immune activation can directly impact autoimmune conditions like Hashimoto’s.
Supporting gut health through a diverse, whole-food diet rich in fiber, fermented foods, and sometimes targeted probiotics and prebiotics, can significantly calm the immune system and reduce flare potential.
4. Infections: Viral, Bacterial, and Fungal
Various infections are suspected of triggering or exacerbating Hashimoto’s flare-ups. Viral infections like Epstein-Barr Virus (EBV), Lyme disease, and even common colds or flu can rev up the immune system, leading to an autoimmune attack on the thyroid. Bacterial infections, such as those caused by H. pylori, and fungal overgrowths can also be problematic.
When the body is fighting off an infection, its immune resources are highly active, which can mistakenly target the thyroid in genetically predisposed individuals. Addressing chronic or recurrent infections is a vital step in managing Hashimoto’s.
5. Nutrient Deficiencies
Several micronutrients are essential for healthy thyroid function and immune regulation. Deficiencies in key vitamins and minerals can contribute to inflammation and increase susceptibility to flare-ups. Common deficiencies include selenium, vitamin D, zinc, iron, and B vitamins, particularly B12.
Selenium is crucial for thyroid enzyme activity and antioxidant defense, while vitamin D plays a significant role in immune modulation. Regular testing to identify deficiencies and then supplementing under the guidance of a healthcare professional is often recommended.
6. Environmental Toxins and Chemical Exposures
Our modern environment exposes us to a myriad of toxins that can burden the immune system and endocrine system. Heavy metals like mercury, lead, and cadmium, as well as pesticides, plastics (BPA), and certain chemicals in personal care products, are believed to contribute to autoimmune development and flares.
Reducing exposure to these toxins by choosing organic foods, filtering water, using natural household cleaners, and supporting the body’s natural detoxification pathways can help alleviate the immune burden.
7. Hormonal Fluctuations
Women are significantly more likely to develop Hashimoto’s, and hormonal shifts often play a role in symptom presentation and flare-ups. Pregnancy, the postpartum period, perimenopause, and menopause are times of profound hormonal change that can influence thyroid function and immune reactivity.
Monitoring thyroid levels closely during these life stages is important, and working with a healthcare provider who understands the interplay between sex hormones and thyroid health can help manage these transitions more smoothly.
8. Overtreatment or Undertreatment of Thyroid Medication
While thyroid hormone replacement is foundational for managing hypothyroidism in Hashimoto’s, getting the dosage just right is critical. Both overtreatment (too much medication) and undertreatment (not enough) can destabilize the thyroid and immune system, potentially leading to a flare-up.
Regular monitoring of TSH, Free T3, and Free T4 levels is essential to ensure your medication dose is optimized for your body’s current needs, preventing both hypothyroid and hyperthyroid symptoms associated with dosage imbalances.
9. Lack of Sleep and Poor Sleep Quality
Sleep is a fundamental pillar of health, especially for the immune system. Chronic sleep deprivation can increase inflammatory markers, disrupt hormone balance (including cortisol), and impair immune regulation, making the body more susceptible to autoimmune flares.
Prioritizing 7-9 hours of quality sleep per night is non-negotiable for managing Hashimoto’s. Establishing a consistent sleep schedule, creating a relaxing bedtime routine, and optimizing your sleep environment can significantly improve immune function and reduce the likelihood of flare-ups.
Proactive Steps to Manage and Prevent Flare-Ups
While identifying triggers is key, proactive management involves a multi-faceted approach. Here are actionable steps:
- Personalized Dietary Adjustments: Work with a functional medicine practitioner or registered dietitian to identify and eliminate trigger foods while ensuring adequate nutrition.
- Stress Management Techniques: Integrate daily practices like meditation, yoga, tai chi, or simply spending time in nature to mitigate stress.
- Optimize Gut Health: Focus on a whole-foods diet, consider bone broth, fermented foods, and targeted supplements to heal and support your gut.
- Address Infections: Work with your doctor to identify and treat any underlying chronic infections that might be burdening your immune system.
- Correct Nutrient Deficiencies: Get tested for key vitamins and minerals and supplement as advised by a healthcare professional.
- Minimize Toxin Exposure: Choose organic foods, use natural personal care products, and ensure clean air and water in your home.
- Regular Thyroid Monitoring: Adhere to your doctor’s recommendations for regular blood tests to ensure your thyroid medication is optimally dosed.
- Prioritize Quality Sleep: Establish a consistent sleep schedule and optimize your bedroom environment for restful sleep.
Managing Hashimoto’s flare-up triggers requires detective work, patience, and a commitment to lifestyle changes. By understanding what can provoke your immune system, you empower yourself to take proactive steps towards greater stability and improved well-being. Always work in close collaboration with your healthcare team to develop a personalized management plan that best suits your individual needs.

