Understanding Hip Bursitis: More Than Just Hip Pain
Hip bursitis, specifically greater trochanteric bursitis, occurs when the bursa (a small, fluid-filled sac that cushions bones, tendons, and muscles around the hip joint) becomes inflamed. This inflammation typically causes pain on the outside of the hip, which can sometimes radiate down the thigh.
The pain often worsens with activity such as walking, running, climbing stairs, or even lying on the affected side. Common causes include repetitive stress, direct trauma, prolonged pressure, and importantly, biomechanical issues like muscle imbalances and poor gait patterns.

The Pivotal Role of Your Gluteus Medius
The gluteus medius is one of three gluteal muscles located on the outer surface of your pelvis. Its primary functions are hip abduction (moving your leg out to the side), internal and external rotation, and crucial pelvic stabilization during activities like walking, running, and standing on one leg.
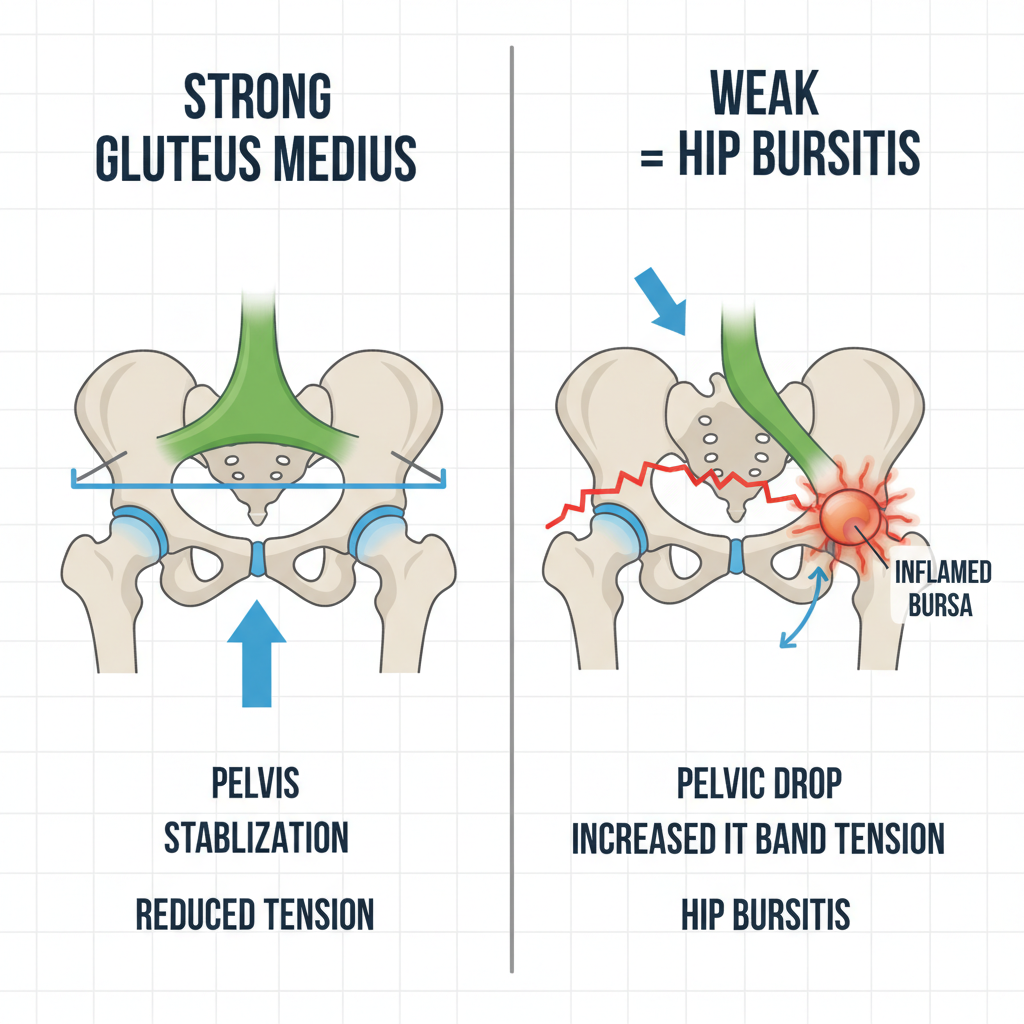
When the gluteus medius is weak or inactive, it can lead to a cascade of biomechanical problems. Without its stabilizing influence, the pelvis tends to drop on the unsupported side during walking (known as a Trendelenburg gait), placing increased stress on the hip joint and the structures surrounding it, including the IT band and the trochanteric bursa.
A weak gluteus medius can cause the iliotibial (IT) band, a thick band of fascia running down the outside of your thigh, to become overly tight. This tightness can rub against the greater trochanter (the bony prominence on the side of your hip), directly irritating the bursa located underneath and contributing significantly to bursitis symptoms.
Why Glute Medius Activation is Essential for Hip Bursitis Recovery
Targeted glute medius activation is not just about strengthening a muscle; it’s about restoring proper hip mechanics and reducing the underlying causes of bursitis. By strengthening this vital muscle, you can:
- Stabilize the Pelvis: A strong glute medius prevents excessive pelvic drop during weight-bearing activities, ensuring better alignment of the hip and lower limb.
- Reduce IT Band Tension: By improving hip abduction and pelvic control, the glute medius helps to alleviate tightness in the IT band, reducing friction over the bursa.
- Decrease Direct Pressure: Better hip alignment and stabilization can reduce direct compressive forces on the greater trochanteric bursa, allowing it to heal.
- Improve Gait and Posture: Enhanced glute medius function leads to a more efficient and less stressful walking pattern, minimizing the repetitive stress that often triggers bursitis.
- Support Long-Term Prevention: Regular activation helps to maintain muscle balance and robust hip mechanics, preventing recurrence of bursitis.
Signs of a Weak Gluteus Medius
Identifying weakness in your gluteus medius is the first step toward effective intervention. Common indicators include:
- Pain on the outside of the hip, especially when standing on one leg.
- A noticeable hip drop on the opposite side when walking or running (Trendelenburg sign).
- Difficulty balancing on one leg.
- Knee pain, often on the outside of the knee, which can be a compensatory issue.
- A “waddling” gait.
You can perform a simple self-assessment by standing on one leg for 30 seconds. If you notice your hip dropping significantly on the side that’s lifted, or if you struggle to maintain balance, it could indicate glute medius weakness.
Principles for Effective Glute Medius Activation
To maximize the benefits of your exercises and prevent further irritation, adhere to these principles:
- Mind-Muscle Connection: Focus on truly engaging the glute medius. Place your hand on the side of your hip to feel the muscle contract.
- Controlled Movements: Avoid swinging or using momentum. Perform each repetition slowly and deliberately.
- Prioritize Form Over Resistance: Incorrect form can engage other muscles or exacerbate your condition. Start with no resistance and add it gradually.
- Gradual Progression: Begin with isometric holds and gentle movements, gradually increasing repetitions, sets, and resistance as your strength improves and pain subsides.
- Pain-Free Range: Never push into pain. If an exercise causes discomfort, modify it or stop.
Top Glute Medius Activation Exercises for Hip Bursitis
These exercises should be performed without pain. If you experience any discomfort, stop and consult a healthcare professional.
Phase 1: Gentle Activation and Awareness
These exercises focus on isolating and waking up the glute medius without putting excessive stress on the bursa.
- Side-Lying Hip Abduction (Clam with Straight Leg): Lie on your unaffected side with your bottom leg slightly bent and your top leg straight and in line with your body. Keeping your hips stacked and your top leg straight, slowly lift your top leg towards the ceiling, leading with your heel. Hold briefly at the top, then slowly lower. Ensure you are not rolling your body backwards.
- Clamshells: Lie on your side with your hips and knees bent to about 45 degrees, feet together. Keeping your feet touching and your core engaged, slowly lift your top knee towards the ceiling, like a clam opening. Keep your pelvis stable and do not let your hips roll back. Slowly lower.
- Hip Bridges: Lie on your back with knees bent and feet flat on the floor, hip-width apart. Engage your core and glutes, lifting your hips off the floor until your body forms a straight line from shoulders to knees. Focus on squeezing your glutes at the top. Slowly lower back down.
Phase 2: Strengthening and Progressive Resistance
Once you can perform Phase 1 exercises pain-free with good form, you can add resistance and complexity.
- Side-Lying Hip Abduction with Resistance Band: Perform the side-lying hip abduction as above, but place a light resistance band around your ankles for added challenge.
- Standing Hip Abduction with Resistance Band: Stand tall with a resistance band around your ankles. Hold onto a wall or chair for balance. Slowly lift one leg out to the side, keeping your body upright and not leaning. Hold briefly, then slowly return to the start. Focus on squeezing the glute medius of the standing leg for stability, and the moving leg for abduction.
- Monster Walks (Lateral Band Walks): Place a resistance band around your ankles or just above your knees. Stand with feet hip-width apart and a slight bend in your knees. Take small, controlled steps sideways, maintaining tension on the band. Keep your hips level and avoid rocking. Walk 10-15 steps in one direction, then switch.
- Single-Leg Balance: Stand on one leg, maintaining a slight bend in your knee and keeping your hips level. Focus on engaging your glute medius on the standing leg to prevent your hip from dropping. Start by holding for 15-30 seconds, progressing to longer durations or with slight upper body movements.
Phase 3: Functional Integration
These exercises integrate glute medius strength into more complex, functional movements.
- Side Plank (Modified): Lie on your side, supporting your body on your forearm and knees (modified) or feet (advanced). Lift your hips off the ground, forming a straight line from head to knees/feet. Focus on engaging your glutes and core to maintain stability.
- Controlled Step-Ups: Step up onto a low step or box, focusing on driving through the heel of your stepping foot. Control the movement, ensuring your knee does not collapse inward. Slowly step back down.
For each exercise, aim for 2-3 sets of 10-15 repetitions, or hold isometric exercises for 30-60 seconds, gradually increasing as tolerated. Listen to your body and prioritize pain-free movement.
Integrating Activation into Your Daily Routine
Consistency is paramount. Aim to perform these exercises 3-5 times a week, ensuring adequate rest days for muscle recovery. Incorporate them into your warm-up routine before other workouts, or as a standalone session. Always stretch gently afterwards.
Holistic Management Strategies for Hip Bursitis
While glute medius activation is vital, a comprehensive approach yields the best results:
- Rest and Activity Modification: Avoid activities that exacerbate your pain. Modify movements to reduce stress on the bursa.
- Ice and Heat Therapy: Apply ice packs to the affected area for 15-20 minutes several times a day to reduce inflammation. Heat may be used before exercises to warm up muscles.
- Stretching: Gently stretch tight muscles, particularly the IT band, piriformis, and hip flexors. Consult a physical therapist for safe and effective stretches.
- Proper Footwear and Orthotics: Ensure your shoes provide good support. Custom orthotics may correct gait imbalances.
- Anti-Inflammatory Medications: Over-the-counter NSAIDs (like ibuprofen) can help manage pain and inflammation, but always consult your doctor.
- Weight Management: If you are overweight, losing excess pounds can significantly reduce stress on your hip joints.
When to Seek Professional Guidance
While glute medius activation can be incredibly beneficial, it’s crucial to consult a healthcare professional for an accurate diagnosis and personalized treatment plan, especially if:
- Your pain is severe or worsening.
- You experience numbness, tingling, or weakness in your leg.
- Your pain does not improve with rest and home remedies.
- Your hip bursitis significantly interferes with your daily activities or sleep.
A physical therapist can assess your specific biomechanics, identify muscle imbalances, and guide you through an appropriate exercise progression, ensuring proper form and maximizing recovery. They can also differentiate hip bursitis from other conditions with similar symptoms.
Conclusion: Empowering Your Hip Health
Hip bursitis can be a frustrating condition, but empowering yourself with knowledge and effective strategies like targeted glute medius activation can pave the way for recovery. By understanding the critical role your gluteus medius plays in hip stability and actively working to strengthen it, you can reduce pain, improve function, and significantly lower your risk of recurrence. Remember to approach your recovery with patience, consistency, and the guidance of healthcare professionals to achieve optimal and lasting hip health.
